|
Diseases of Poultry
By Ivan Dinev, DVM, PhD
|
HAEMORRHAGIC ENTERITIS OF TURKEYS


187.188.The haemorrhagic enteritis (HE) is an acute viral disease in young turkeys, characterized by a sudden onset, bloody faeces and various, but often high death rate. Blood discharge from the vent (187), fresh blood in faeces or melena (188) could be observed.
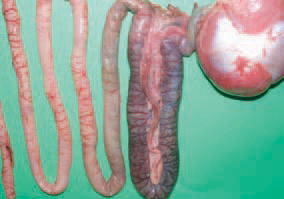
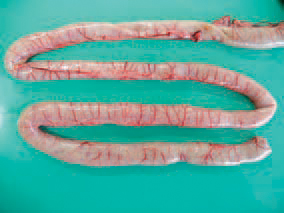
189.190.HE is observed in turkeys at the age of 6 - 11 weeks but most commonly at the age of 7 - 9 weeks. As an exception, HE could be observed in turkeys under 4 weeks of age, presumably due to maternal antibodies. The small intestine, especially the duodenum, has a dark red colour and ramiform blood vessels prominating under the serous coat, and sometimes, haemorrhages are seen through the intestinal wall.
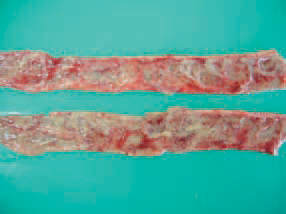

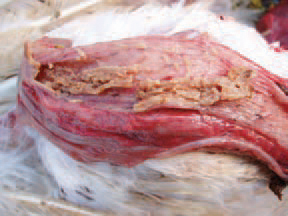
191.192.193.HE is characterized by rapidly progressing clinical signs and disease course of about 10 days. The peak death rate is reached by the middle of the period. The entire death rate varies between 2-3% and 5-10% but could reach 60% as well. The turkeys are depressed, a sharp reduction in forage and water consumption is seen. The extent of lesions of the interstitial mucosa varies from hyperaemic to haemorrhagic (191), severe haemorrhagic or fibrinous necrotic inflammation (192 & 193).
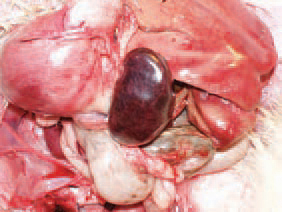
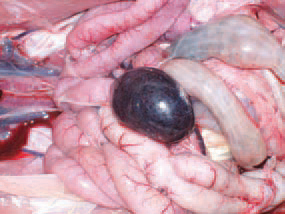
194.195.The spleen of infected birds is typically enlarged, haemorrhagic, crumbly, motted or marble-like. The aetiological agent of HE is an adenovirus of group (type) II (HEV). The viruses or marble spleen disease in pheasants (MSDV) and avian adenvirus splenimegaly (AAS) that are serglogically similar, beling to the same group.
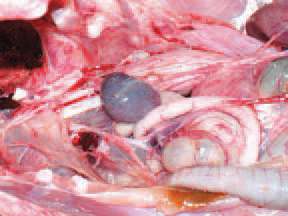
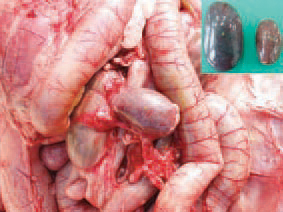
196.197.Later, the spleen reduces its size 2-3 times and acquires a specific silvery-grey colour. The serological studies show that HEV is widely distributed among adult turkeys. There is no evidence for vertical transmission. HEV is spread horizontally by ingestion of faeces of infected turkeys. Contaminated litter, equipment, shoes, other birds, rodents etc. are also important in the transmission of the infection.
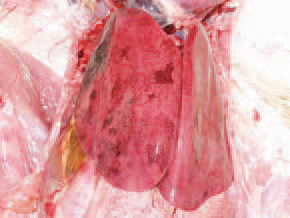
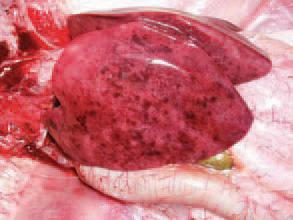
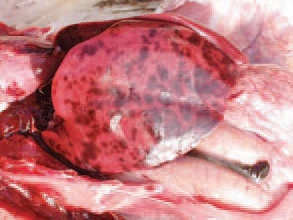
198.199.200.The liver is enlarged, crumbly and mottled with multiple haemorrhages, varying from petechiae to ecchymoses. Dead birds are in a good condition, with pale skin. Once having appeared in the farm, the infection is often recurring in other flocks. The HEV infection in turkeys results in a transient immunosuppression and consequently, a secondary E. coli septicaemia
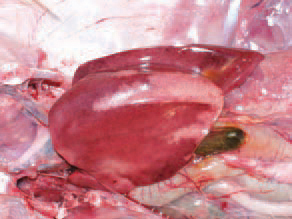
201Less frequently, extensive necrotic foci, sometimes haemorrhagically infarcted, could be detected in the liver.
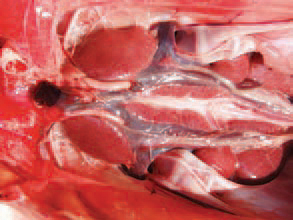
202The kidneys are enlarged and haemorrhagic.
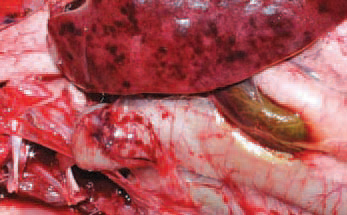
203In many instances, the small intestinal and gastric serous coats are encompassed by petechial or striated haemorrhages.
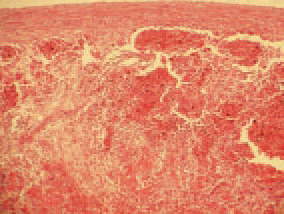
204., hyperplasia of the white spleen pulp, necroses, subcapsular and periarteriolar haemorrhages are observed.
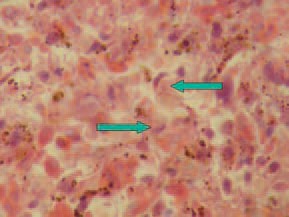
205.A characteristic diagnostic sign is the discovery of large acidophilic, rarely basophilic intra-nuclear inclusion bodies in the reticuloendothelial cells. The displaced and condensed nuclear chromatin pattern around the inclusion bodies often looks like a crescent.
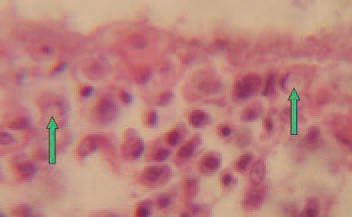
206Similar inclusion bodies could be sometimes found out in lamina propria of the intestinal mucosa.
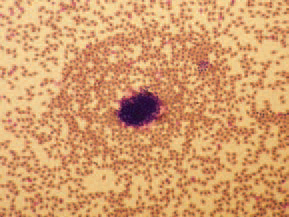
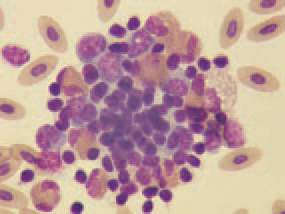
207.208.The staining of peripheral blood smears reveals a picture, characte-ristic for septicaemia. The typical gross lesions and the history of the disease allow making a tentative diagnosis for HE. The histological detection of intranuclear inclusion bodies in the reticuloendothelial cells of the spleen or intestines confirms the diagnosis. For identification of the HEV, the agar gel precipitation method could be used. The viral antigen could be detected in fresh or frozen spleen tissue, diluted 1:1 with saline or in sera obtained from diseased turkeys. HE should be distinguished from other cases of severe enteritis in turkeys, acute E. coli septicaemia and some other septicaemic states (streptococcosis, fowl cholera etc.). Within weeks after the beginning of the disease, an appropriate antibiotic therapy should be initiated for prevention of secondary E. coli septicaemia. Practically, there is no effective therapy for HE in turkeys.






